
Digital Transformation in Healthcare: 2026 Guide
Quick Summary: Digital transformation in healthcare integrates advanced technologies like AI, EHR systems, telemedicine, and data analytics to revolutionize patient care delivery, operational efficiency, and clinical outcomes. According to HHS and CMS initiatives, these innovations enable real-time data access, predictive analytics, and personalized treatment while reducing costs and administrative burdens. The transformation requires strategic planning, regulatory compliance, workforce training, and patient-centered approaches to overcome implementation challenges.
Healthcare stands at a technological crossroads. The industry that once relied on paper charts and face-to-face consultations now harnesses artificial intelligence to predict patient outcomes and delivers care through smartphones.
But digital transformation isn't just about adopting new gadgets. It represents a fundamental restructuring of how healthcare organizations deliver value to patients, manage operations, and compete in an increasingly complex marketplace.
The shift gained momentum through government initiatives. The Centers for Medicare & Medicaid Services (CMS) and the Office of the National Coordinator for Health Information Technology (ONC) established regulations defining meaningful use of electronic health records, creating financial incentives for hospitals and providers to modernize their systems. According to ONC data, as of 2021, 96% of all non-federal acute care hospitals and nearly 4 out of 5 office-based physicians (78%) in the U.S. had adopted a certified EHR.
More recently, the Department of Health and Human Services announced on December 19, 2025, a Request for Information to harness artificial intelligence in clinical care. The initiative aims to use regulation, reimbursement, and research levers to enable AI adoption and reduce healthcare costs while improving patient outcomes.
This transformation touches every corner of healthcare delivery. From rural clinics implementing telemedicine platforms to major hospital systems deploying predictive analytics, the technology landscape continues evolving at breakneck speed.
What Digital Transformation Actually Means in Healthcare
Digital transformation goes beyond installing new software or purchasing tablets for clinicians. It represents a comprehensive reimagining of healthcare delivery models, operational workflows, and patient engagement strategies.
At its core, the transformation involves integrating digital technologies into all areas of healthcare operations. This fundamentally changes how organizations operate and deliver value to patients. It's also a cultural change that requires organizations to continually challenge the status quo, experiment, and become comfortable with failure.
The Electronic Health Record (EHR) serves as a foundational element. According to CMS, an EHR is an electronic version of a patient's medical history maintained by the provider over time. It includes all key administrative clinical data relevant to that person's care, including demographics, progress notes, problems, medications, vital signs, past medical history, immunizations, laboratory data, and radiology reports.
But here's the thing—EHRs represent just the beginning. True transformation encompasses telemedicine platforms, wearable health devices, artificial intelligence for diagnostics, blockchain for secure data sharing, and Internet of Things (IoT) sensors for remote patient monitoring.
The Technology Stack Driving Change
Modern healthcare organizations deploy an interconnected ecosystem of technologies. These tools work together to create seamless experiences for patients and providers alike.
Cloud computing provides scalable infrastructure for storing massive amounts of health data while ensuring accessibility from any location. This became particularly critical during the pandemic when remote work became necessary for many healthcare administrative functions.
Data analytics platforms process information from multiple sources to identify patterns, predict outcomes, and support clinical decision-making. According to TierPoint research, 65% of U.S. hospitals have led to the use of AI-assisted predictive tools embedded in their EHR systems, enabling faster and more informed decision-making.
Telemedicine solutions connect patients with providers across distances, eliminating geographic barriers to care. Mobile health applications extend care beyond clinical settings, empowering patients to monitor conditions, track medications, and communicate with care teams.
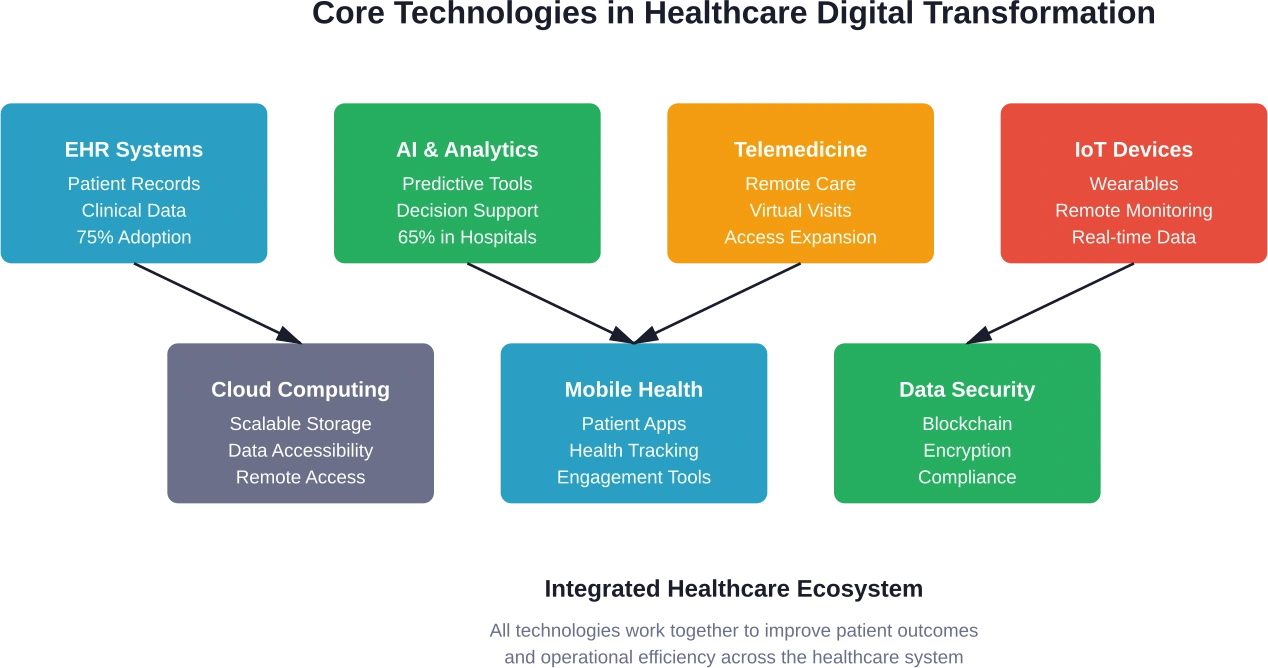
Key Benefits Driving Healthcare Digital Transformation
Healthcare organizations pursue digital transformation for concrete, measurable benefits. The most frequently cited outcomes reveal what matters most to health systems and their patients.
According to research, 92% of health systems identify better patient experience as their top desired outcome from digital transformation. This focus makes sense—patient satisfaction directly impacts outcomes, compliance with treatment plans, and institutional reputation.
Improved Patient Outcomes and Care Quality
Digital technologies enable more accurate diagnoses and personalized treatment plans. AI-powered diagnostic tools analyze medical images with precision that matches or exceeds human specialists in certain applications. Predictive analytics identify patients at high risk for complications, allowing proactive interventions.
Real-time data access transforms clinical decision-making. When providers access complete patient histories, test results, and medication lists instantly, they make better-informed choices. This reduces medical errors, prevents adverse drug interactions, and eliminates redundant testing.
Remote monitoring through connected devices catches deteriorating conditions before they become emergencies. Patients with chronic conditions like diabetes, heart failure, or COPD benefit particularly from continuous monitoring that alerts care teams to concerning trends.
Operational Efficiency and Cost Reduction
Digital transformation delivers substantial operational improvements. Automated workflows reduce administrative burdens, freeing staff to focus on patient care rather than paperwork. Electronic prescribing eliminates handwriting interpretation errors and speeds pharmacy fulfillment.
The benefits include increased employee productivity, improved efficiency and effectiveness of health unit operations, and reduced operating costs. These savings compound over time as systems optimize and workflows mature.
Inventory management systems prevent medication stockouts and reduce waste from expired supplies. Scheduling optimization reduces appointment gaps and minimizes patient wait times. Revenue cycle management platforms accelerate billing and collections while reducing claim denials.
Enhanced Access and Patient Engagement
Telemedicine breaks down geographic barriers to specialist care. Rural patients access subspecialists without traveling hundreds of miles. Mobility-impaired individuals receive care without transportation challenges. Working patients schedule appointments outside traditional office hours.
Patient portals empower individuals to take active roles in their health management. They review test results, request prescription refills, communicate with providers, and access educational resources. This transparency builds trust and improves adherence to treatment recommendations.
Mobile applications extend engagement beyond clinic visits. Medication reminders reduce missed doses. Symptom trackers help patients recognize patterns. Educational content answers questions at the point of need.
|
Benefit Category |
Key Improvements |
Impact Metrics |
|---|---|---|
|
Patient Experience |
Better access, personalized care, improved communication |
92% of systems prioritize this outcome |
|
Clinical Outcomes |
Accurate diagnoses, predictive analytics, proactive interventions |
Reduced errors, better patient safety |
|
Operational Efficiency |
Automated workflows, optimized scheduling, inventory management |
Lower costs, increased productivity |
|
Data-Driven Decisions |
Real-time analytics, predictive tools, population health insights |
65% of hospitals use AI-assisted tools |
|
Access Expansion |
Telemedicine, remote monitoring, mobile health apps |
Geographic barriers eliminated |
Plan and Estimate Your Healthcare App with OSKI
Digital transformation in healthcare often comes down to one thing - building software that actually fits real workflows, compliance needs, and patient experience. That’s where working with a development team early in the planning stage makes a difference.
OSKI Solutions helps healthcare teams turn ideas into clear technical scopes and realistic cost estimates before development starts. Instead of guessing budgets, you get a structured breakdown of what your app will require and how long it will take.
With OSKI, you can:
- define features based on real use cases
- get a clear cost estimate before development
- understand timelines and technical requirements
Get a clear plan and cost for your healthcare app - talk to OSKI Solutions.
Transform Healthcare with Digital Innovation
Modernize healthcare systems with secure, scalable digital solutions. From patient platforms and telehealth to data analytics and automation, we help healthcare providers improve efficiency and patient outcomes.
Government Initiatives Shaping Digital Healthcare
Federal regulations and incentive programs accelerated healthcare's digital transformation. Understanding these initiatives helps organizations align strategies with regulatory requirements and funding opportunities.
The HITECH Act and Meaningful Use
The Health Information Technology for Economic and Clinical Health (HITECH) Act, passed as part of the American Recovery and Reinvestment Act of 2009, fundamentally changed healthcare IT adoption. The Act provided incentive payments for the adoption and meaningful use of certified EHR technology.
CMS and ONC established complementary regulations defining meaningful use standards. The Medicare EHR incentive program provided payments to eligible professionals, eligible hospitals, and critical access hospitals demonstrating meaningful use of certified technology.
Under Medicaid, critical access hospitals were included in the definition of acute care hospitals for incentive program eligibility. The Recovery Act amended the Medicaid statute to provide 100 percent Federal financial participation for these incentive payments.
Economic analysis of the final rules estimated that incentive payments under Medicare and Medicaid EHR programs for 2011 through 2019 would range from $9.7 billion to $27.4 billion, driving widespread adoption across the industry.
AI in Clinical Care: The 2025 HHS Initiative
On December 19, 2025, HHS announced a Request for Information seeking public input on harnessing artificial intelligence as part of clinical care. This initiative represents the next evolution in healthcare digital transformation policy.
The RFI focuses on how HHS can use regulation, reimbursement, and research and development levers to enable AI adoption and use in clinical care. The stated goals include deflating healthcare costs while improving health outcomes—a dual mandate that reflects growing pressure to control spending without sacrificing quality.
This initiative signals federal commitment to AI as a core component of healthcare delivery, not merely an experimental technology. It creates a framework for providers to invest in AI tools with confidence that regulatory and reimbursement structures will support their use.
Certification and Standards
ONC established certification programs for health information technology to ensure systems meet technical standards for functionality, security, and interoperability. The ONC Health IT Certification Program was established through the HITECH Act in 2009, with the Initial Set of Standards, Implementation Specifications, and Certification Criteria published in 2010.
These standards ensure different systems can exchange information effectively. Interoperability remains critical—patient data locked in proprietary systems delivers limited value. Standards-based data exchange enables care coordination across organizations and specialties.
Implementation Challenges and How to Overcome Them
Digital transformation sounds compelling in theory. But implementation proves far more complex than purchasing software licenses and flipping a switch.
Organizations encounter predictable obstacles. Recognizing these challenges early allows proactive mitigation strategies.
Legacy System Integration
Healthcare organizations rarely start with blank slates. Decades of accumulated technology create complex environments with disparate systems that don't communicate effectively.
Legacy electronic medical record systems may lack modern APIs for integration. Departmental systems operate in isolation. Medical devices use proprietary data formats. Creating a unified digital ecosystem requires extensive integration work.
Successful organizations approach integration strategically. They inventory existing systems, identify critical data flows, and prioritize integration projects based on clinical and operational impact. Middleware platforms can bridge communication gaps between incompatible systems.
Sometimes the best approach involves replacing obsolete systems rather than attempting integration. The cost-benefit analysis should consider ongoing maintenance expenses, security vulnerabilities, and opportunity costs of delayed transformation.
Change Management and Workforce Adaptation
Technology implementation fails without user adoption. Healthcare workers accustomed to established workflows resist changes that disrupt familiar patterns, particularly when new systems add complexity or slow clinical processes.
Physicians especially resist technology that interferes with patient interaction. If EHR systems require extensive data entry during encounters, providers perceive them as barriers rather than tools.
Effective change management starts with stakeholder engagement during planning phases. When end users help design workflows and select systems, they develop ownership of solutions. Training must be comprehensive, role-specific, and available as ongoing support rather than one-time events.
Organizations should identify clinical champions—respected providers who embrace new technologies and model effective use. Peer influence often proves more powerful than administrative mandates.
Data Security and Privacy Concerns
Healthcare data represents prime targets for cybercriminals. Protected health information sells for high prices on dark web markets. Ransomware attacks can shut down entire hospital systems, threatening patient safety.
Digital transformation expands attack surfaces. More connected devices mean more potential entry points for hackers. Cloud systems require different security approaches than on-premise infrastructure. Mobile applications introduce vulnerabilities if not properly secured.
Compliance with HIPAA and other privacy regulations adds complexity. Organizations must implement technical safeguards, establish security policies, train workforce members, and document compliance activities.
Security cannot be an afterthought. It must be embedded in digital transformation planning from the beginning. This includes encryption for data at rest and in transit, multi-factor authentication, regular security audits, incident response planning, and continuous monitoring for threats.
Cost and Resource Constraints
Digital transformation requires significant investment. Software licensing, hardware infrastructure, integration services, training, and ongoing maintenance add up quickly. Many healthcare organizations operate on thin margins, making large technology investments difficult to justify.
The business case must demonstrate clear ROI. This requires quantifying benefits like reduced readmissions, improved coding accuracy, decreased administrative costs, and enhanced patient satisfaction. Spreading implementations across multiple phases can make investments more manageable.
Cloud-based solutions offer alternatives to large capital expenditures. Subscription pricing converts major upfront costs into predictable operational expenses. This approach also eliminates infrastructure management responsibilities.
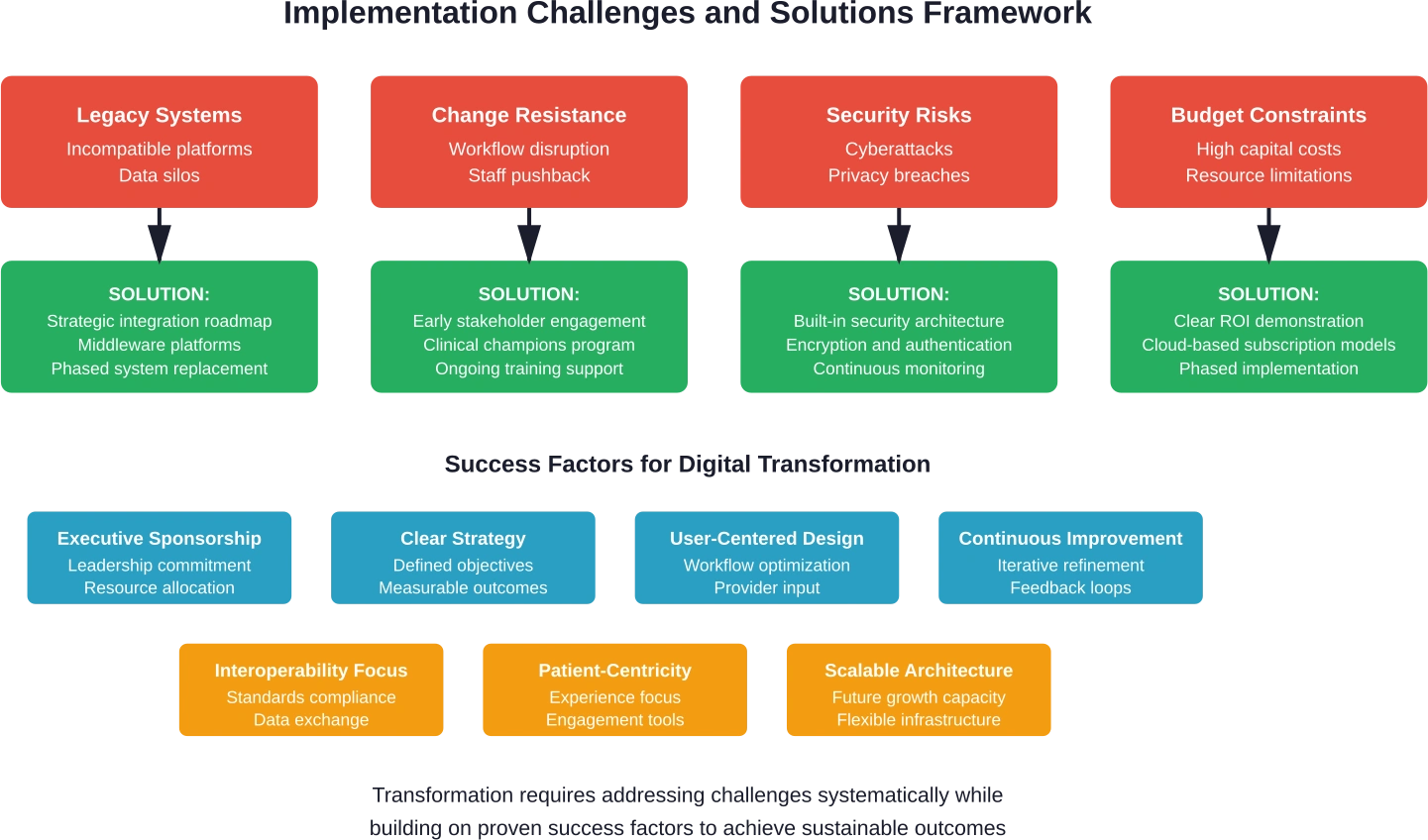
The Role of Artificial Intelligence in Healthcare
Artificial intelligence represents perhaps the most transformative technology in healthcare's digital evolution. Its applications extend across clinical care, operational management, and research.
Clinical Decision Support and Diagnostics
AI algorithms analyze medical images with remarkable accuracy. Radiology applications detect abnormalities in X-rays, CT scans, and MRIs. Pathology systems identify cancer cells in tissue samples. Ophthalmology tools screen for diabetic retinopathy and other retinal diseases.
These systems don't replace physicians—they augment human expertise. Radiologists use AI as a second opinion, catching findings they might otherwise miss. The technology proves particularly valuable in areas with specialist shortages.
Predictive analytics identify patients at high risk for specific conditions. Algorithms analyze electronic health records to flag individuals likely to develop sepsis, experience readmissions, or suffer adverse events. Early identification enables preventive interventions that improve outcomes and reduce costs.
Operational Applications
Beyond clinical care, AI optimizes healthcare operations. Natural language processing extracts information from physician notes, automating coding and documentation tasks. This reduces administrative burdens while improving billing accuracy.
Scheduling algorithms optimize appointment slots based on historical patterns, reducing no-shows and gaps. Supply chain systems predict demand for medications and supplies, preventing stockouts while minimizing excess inventory.
Chatbots and virtual assistants handle routine patient inquiries, schedule appointments, and provide basic health information. This frees staff for complex tasks requiring human judgment while improving patient access to information.
Federal Support for AI Adoption
The HHS Request for Information announced in December 2025 signals strong federal support for AI integration in healthcare. The initiative explores how regulation, reimbursement, and research funding can enable AI adoption while ensuring safety and effectiveness.
This regulatory clarity matters. Healthcare organizations hesitate to invest heavily in technologies with uncertain reimbursement or regulatory pathways. Federal guidance reduces this uncertainty, accelerating adoption.
The dual mandate—reducing costs while improving health outcomes—reflects realistic expectations for AI. The technology must deliver tangible value, not just impressive technical capabilities.
Telemedicine and Remote Patient Monitoring
The pandemic accelerated telemedicine adoption by years, perhaps decades. What seemed experimental in 2019 became standard practice by 2020. This rapid deployment demonstrated both the potential and challenges of virtual care delivery.
Virtual Care Models
Telemedicine encompasses diverse delivery models. Synchronous video visits replicate traditional appointments in virtual settings. Asynchronous store-and-forward systems allow specialists to review images and data without real-time interaction. Remote patient monitoring uses connected devices to track vital signs and symptoms continuously.
Each model suits different clinical scenarios. Primary care often works well via video visits. Dermatology frequently uses store-and-forward approaches for lesion evaluation. Chronic disease management benefits from continuous remote monitoring.
Hybrid models combine virtual and in-person care. Patients might have initial consultations in person, then conduct follow-ups virtually. Complex cases requiring physical examination happen in clinics, while routine check-ins occur remotely.
Breaking Down Access Barriers
Telemedicine transforms access in underserved areas. Rural communities often lack specialist physicians. Virtual consultations connect patients with subspecialists hundreds of miles away, eliminating travel burdens and associated costs.
Mobility limitations no longer prevent medical appointments. Elderly patients, individuals with disabilities, and those without reliable transportation access care from home. This proves particularly valuable for mental health services, where stigma sometimes prevents clinic visits.
Extended hours become feasible. Virtual urgent care operates evenings and weekends without the overhead of staffing physical facilities. Patients resolve minor issues quickly rather than waiting for office hours or visiting emergency departments unnecessarily.
Quality and Reimbursement Considerations
Early concerns about telemedicine quality have largely been addressed. Research demonstrates comparable outcomes for many conditions when delivered virtually versus in-person. Patient satisfaction typically runs high, particularly regarding convenience and access.
Reimbursement parity remains important for sustainable telemedicine programs. When virtual visits receive significantly lower payment than in-person encounters, providers lack financial incentives to offer them. Many payers now reimburse telemedicine at rates comparable to traditional visits, supporting continued availability.
Data Analytics and Population Health Management
Healthcare generates massive amounts of data. Electronic health records, claims systems, wearable devices, patient-reported outcomes, and genomic sequencing all contribute to growing data repositories. The challenge lies in transforming this data into actionable insights.
From Data to Intelligence
Data analytics platforms integrate information from disparate sources, creating comprehensive views of patient populations. This aggregated data reveals patterns invisible in individual records.
Population health management identifies cohorts requiring intervention. Analytics might reveal patients with diabetes showing early signs of complications, enabling proactive outreach. Or flag individuals overdue for cancer screenings, prompting reminders.
Stratification algorithms categorize patients by risk level. High-risk individuals receive intensive care coordination. Moderate-risk patients get targeted interventions. Low-risk populations require only routine preventive care. This resource allocation improves outcomes while controlling costs.
Predictive and Prescriptive Analytics
Predictive analytics forecast future events based on historical patterns. Models predict which patients will likely experience readmissions, develop complications, or fail to adhere to treatment plans. These predictions enable preventive actions.
Prescriptive analytics go further, recommending specific interventions. Rather than simply identifying high-risk patients, systems suggest optimal treatment approaches based on similar patient outcomes. This precision medicine approach personalizes care to individual characteristics.
Real-time analytics support clinical decision-making at the point of care. When prescribing medications, systems check for interactions, suggest evidence-based alternatives, and flag cost-effective options. These interventions improve safety and efficiency without disrupting workflows.
Quality Improvement and Benchmarking
Analytics platforms track quality metrics across organizations and providers. Dashboards display performance on measures like readmission rates, patient satisfaction scores, and clinical outcome indicators.
Benchmarking comparisons reveal variation in performance. When some providers achieve significantly better outcomes than peers treating similar patients, analytics identify best practices worth spreading. This drives continuous quality improvement.
Transparency in quality data increasingly influences patient choices and payer contracts. Organizations demonstrating superior outcomes attract more patients and negotiate better reimbursement rates. This creates positive incentives for quality improvement.
Patient Engagement and Experience Technologies
Digital transformation fundamentally changes how patients interact with healthcare systems. Passive recipients of care become active participants in health management.
Patient Portals and Mobile Applications
Patient portals provide secure access to health information. Patients review test results, medication lists, and visit summaries. They request prescription refills, schedule appointments, and message care teams with questions.
This transparency empowers informed decision-making. When patients understand their conditions and treatment options, they make choices aligned with their values and preferences. Engagement improves adherence to treatment plans.
Mobile applications extend functionality beyond portals. Symptom checkers guide users through decision trees, recommending appropriate care settings. Medication trackers send reminders and record doses taken. Health coaching apps provide education and motivation for behavior change.
Wearables and Personal Health Devices
Consumer wearables track activity, sleep, heart rate, and other metrics. While initially marketed for fitness, these devices increasingly serve medical purposes. Atrial fibrillation detection through smartwatch ECG features demonstrates the blurring line between consumer and medical devices.
Medical-grade devices enable home monitoring of chronic conditions. Connected glucose meters transmit readings directly to care teams. Blood pressure cuffs send measurements to physicians. Weight scales track fluid retention in heart failure patients.
Integration of device data with electronic health records closes the loop. Physicians view continuous monitoring data alongside lab results and clinic notes, creating comprehensive pictures of patient status between appointments.
Shared Decision-Making Tools
Digital tools support shared decision-making between patients and providers. Decision aids present treatment options with evidence-based information about benefits, risks, and alternatives. Interactive formats help patients clarify preferences and values.
These tools prove particularly valuable for preference-sensitive decisions where multiple reasonable options exist. Cancer treatment choices, elective surgical procedures, and chronic disease management approaches often involve tradeoffs between outcomes patients value differently.
Research in patient-physician communication highlights how health IT promotes empowerment and collaborative decision-making. However, challenges around usability and ensuring tools enhance rather than complicate interactions remain important considerations.
|
Technology Type |
Primary Functions |
Key Benefits |
Considerations |
|---|---|---|---|
|
Patient Portals |
Records access, messaging, scheduling, refills |
Transparency, convenience, engagement |
Digital literacy requirements, access barriers |
|
Mobile Health Apps |
Symptom tracking, education, reminders, coaching |
Continuous engagement, behavior change support |
Quality variation, privacy concerns |
|
Wearable Devices |
Activity tracking, vital signs monitoring, alerts |
Continuous data, early detection, prevention |
Data accuracy, integration challenges |
|
Telehealth Platforms |
Virtual visits, remote monitoring, consultations |
Access expansion, convenience, cost reduction |
Technology requirements, reimbursement |
|
Decision Aids |
Treatment information, preference clarification |
Informed choices, aligned decisions |
Adoption by providers, integration workflows |
Addressing Health Disparities Through Digital Transformation
Digital health technologies promise expanded access and improved outcomes. But they also risk widening existing health disparities if not implemented thoughtfully.
The Digital Divide Challenge
Not everyone has equal access to technology. Broadband internet remains unavailable in many rural areas. Lower-income households may lack smartphones or computers. Older adults often struggle with digital literacy.
When healthcare delivery shifts toward digital channels, populations without technology access get left behind. A telemedicine program that improves access for some while excluding others exacerbates rather than reduces disparities.
Research on digital evolution and healthcare inequalities shows that digitalization can generate new forms of inequality. Although literature on this topic remains limited, growing attention focuses on understanding and addressing these challenges.
Strategies for Equitable Access
Healthcare organizations must proactively address access barriers. This includes maintaining non-digital options for populations unable or unwilling to use technology. Phone-based appointment scheduling, paper forms, and in-person services remain necessary.
Technology assistance programs help bridge divides. Providing tablets or hotspots to underserved patients enables participation in virtual care. Digital navigators help individuals learn to use patient portals and health apps. These support services prove critical for equitable implementation.
Design choices impact accessibility. Applications with simple interfaces, large fonts, and multilingual support serve broader populations. Voice-enabled interactions help users with limited literacy or visual impairments.
Cultural and Language Considerations
Effective digital health tools reflect diverse populations' needs. Translation services must extend beyond simple language conversion to culturally appropriate content that resonates with different communities.
Community engagement during design phases ensures solutions address real needs rather than assumptions. When developers understand specific barriers and preferences different populations face, they create more effective and acceptable tools.
The Future Landscape of Digital Healthcare
Digital transformation continues accelerating. Emerging technologies promise further disruption and innovation in how healthcare gets delivered.
Artificial Intelligence Evolution
AI capabilities will expand beyond current applications. Generative AI may assist with clinical documentation, creating visit summaries from conversation analysis. Multimodal AI combining imaging, genomics, and clinical data could enable more accurate diagnoses and personalized treatment recommendations.
Drug discovery increasingly leverages AI to identify promising compounds and predict their effects. This could dramatically shorten development timelines and reduce costs, potentially making treatments for rare diseases economically viable.
The HHS focus on AI for cost reduction and health improvement signals sustained federal support. As algorithms prove their value and regulatory frameworks mature, adoption will accelerate across the healthcare ecosystem.
Internet of Medical Things Expansion
Connected medical devices will proliferate. Implantable sensors could monitor biochemical markers continuously, alerting providers to concerning changes before symptoms appear. Smart pills with embedded sensors might track medication ingestion and internal conditions.
Home becomes a primary care delivery site for many services. Remote monitoring technology enables hospital-level surveillance in residential settings. This shift reduces costly institutional care while improving patient comfort and satisfaction.
Research on Artificial Intelligence of Things (AIoT) in healthcare demonstrates how combining connectivity with intelligence creates self-reinforcing ecosystems where improvements in any dimension enhance outcomes across all areas.
Precision Medicine and Genomics
Genomic sequencing costs continue declining, making precision medicine approaches increasingly accessible. Treatment selection based on genetic profiles rather than population averages improves efficacy while reducing adverse effects.
Pharmacogenomics predicts drug responses based on genetic variations. This eliminates trial-and-error prescribing for conditions like depression where multiple medication options exist but individual responses vary dramatically.
Cancer treatment increasingly relies on tumor genomic profiling to select targeted therapies. As understanding of genetic drivers improves and targeted treatments expand, outcomes continue improving for previously difficult-to-treat malignancies.
Blockchain for Data Security and Interoperability
Blockchain technology offers solutions for healthcare data challenges. Distributed ledger systems could enable secure health information exchange while maintaining patient control over data access. This addresses both privacy concerns and interoperability barriers.
Smart contracts might automate prior authorizations and claims processing, reducing administrative burden. Pharmaceutical supply chain tracking using blockchain could prevent counterfeit medications and improve safety.
While still emerging, blockchain applications in healthcare warrant attention as potential solutions to persistent challenges around data security, patient consent, and system interoperability.
Building a Digital Transformation Strategy
Successful digital transformation requires strategic planning, not tactical technology purchases. Organizations need comprehensive roadmaps aligned with clinical and business objectives.
Assessment and Prioritization
Transformation begins with honest assessment of current state. What technologies already exist? Where do workflows break down? What patient and provider pain points need addressing?
Gap analysis identifies differences between current capabilities and desired future state. This reveals priorities for investment and improvement. Not all gaps require immediate attention—strategic planning sequences initiatives based on impact and feasibility.
Stakeholder input proves essential. Clinicians understand workflow challenges technology should solve. Patients identify access barriers and engagement obstacles. IT staff know technical constraints and integration requirements. Executive leadership provides strategic direction and resource allocation authority.
Phased Implementation Approach
Big bang implementations rarely succeed in complex healthcare environments. Phased approaches reduce risk while enabling learning between stages.
Pilot programs test technologies and workflows with limited user groups before enterprise rollout. Early feedback identifies issues requiring correction. Success stories from pilots build momentum and reduce resistance for broader deployment.
Quick wins demonstrate value early, building support for longer-term initiatives. Selecting initial projects with high visibility and clear benefits creates positive momentum. Success breeds enthusiasm that carries through more challenging later phases.
Measuring Success
Digital transformation requires clear success metrics. These should tie directly to strategic objectives rather than measuring technology adoption for its own sake.
Clinical outcome metrics might include readmission rates, infection rates, or patient safety indicators. Operational measures could track throughput, cycle times, or resource utilization. Financial metrics include cost per case, days in accounts receivable, or revenue per provider.
Patient experience metrics increasingly matter. Satisfaction scores, Net Promoter Scores, and patient-reported outcome measures capture the patient perspective on transformation initiatives.
Regular review of metrics enables course correction. If initiatives aren't delivering expected benefits, organizations must diagnose why and adjust approaches. Measurement without action wastes resources.
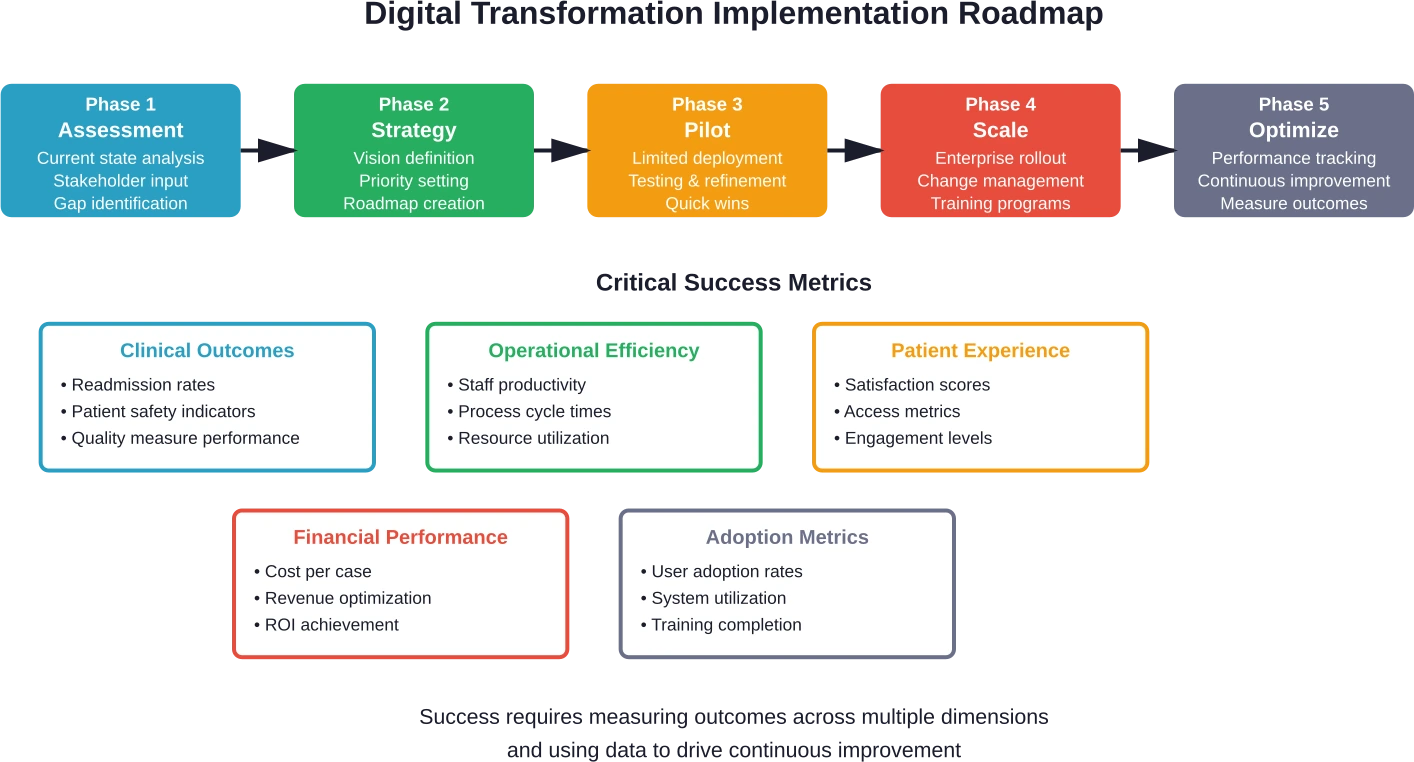
Frequently Asked Questions
What is digital transformation in healthcare?
Digital transformation in healthcare involves integrating advanced technologies like electronic health records, artificial intelligence, telemedicine, data analytics, and mobile applications into all aspects of healthcare delivery. It fundamentally changes how organizations operate, deliver patient care, and create value. According to government initiatives from HHS and CMS, this transformation aims to improve patient outcomes, reduce costs, enhance access, and increase operational efficiency through meaningful use of certified health information technology.
What are the main benefits of healthcare digital transformation?
Research shows that 92% of health systems identify better patient experience as their top desired outcome. Additional benefits include improved clinical outcomes through AI-assisted diagnostics and predictive analytics (used by 65% of U.S. hospitals), enhanced operational efficiency with increased staff productivity and reduced costs, expanded access through telemedicine that eliminates geographic barriers, and data-driven decision-making with real-time analytics. The transformation also supports proactive population health management and personalized treatment approaches.
How does AI fit into healthcare digital transformation?
Artificial intelligence plays a central role in modern healthcare transformation. HHS announced in December 2025 a Request for Information on using AI to reduce healthcare costs and improve outcomes. AI applications include clinical decision support, medical image analysis, predictive analytics for patient risk stratification, natural language processing for documentation automation, operational optimization for scheduling and resource allocation, and drug discovery acceleration. The technology augments rather than replaces human expertise, improving accuracy and efficiency across clinical and operational domains.
What challenges do healthcare organizations face during digital transformation?
Common challenges include integrating legacy systems that use incompatible technologies and proprietary data formats, managing change resistance from staff accustomed to established workflows, ensuring data security and privacy compliance in increasingly connected environments, addressing budget constraints given significant upfront and ongoing costs, and overcoming the digital divide to prevent widening health disparities. Successful organizations address these challenges through strategic planning, stakeholder engagement, phased implementation, and dedicated change management programs.
How is telemedicine changing healthcare delivery?
Telemedicine fundamentally expands healthcare access by eliminating geographic barriers to specialist care, accommodating mobility-impaired patients, extending service hours beyond traditional clinic times, and reducing costs associated with facility overhead and patient travel. Virtual care models include synchronous video visits, asynchronous store-and-forward consultations, and remote patient monitoring using connected devices. Research demonstrates comparable outcomes for many conditions when delivered virtually versus in-person, with high patient satisfaction particularly regarding convenience and access.
What role do patient engagement technologies play?
Patient engagement technologies transform individuals from passive care recipients to active health managers. Patient portals provide secure access to medical records, test results, and communication with care teams. Mobile applications offer medication reminders, symptom tracking, and health education. Wearable devices enable continuous monitoring of vital signs and activity levels. These technologies improve treatment adherence, support shared decision-making, enable early detection of concerning trends, and empower patients with information and tools to manage their health between clinical encounters.
How can healthcare organizations ensure equitable access during digital transformation?
Addressing health equity requires proactive strategies including maintaining non-digital options for populations without technology access, providing devices and internet connectivity to underserved patients, offering digital navigation support to help individuals learn new tools, designing applications with accessibility features like simple interfaces and multilingual support, engaging communities during planning to understand specific barriers and preferences, and continuously monitoring for disparities in access and outcomes. Research shows that digitalization can generate inequalities if not implemented thoughtfully with equity as a core consideration.
Conclusion
Digital transformation represents the most significant shift in healthcare delivery since the advent of modern medicine. Technologies once considered experimental—artificial intelligence, telemedicine, predictive analytics, remote monitoring—now form the foundation of how healthcare organizations operate and compete.
The transformation delivers measurable benefits. According to research cited in competitor content, 75% of U.S. hospitals use electronic health records, dramatically improving data accessibility and care coordination. According to digital transformation industry analysis, 65% of hospitals have adopted AI-assisted predictive tools, enabling faster and more informed clinical decisions. Health systems report that 92% prioritize better patient experience as their primary transformation objective.
Federal support accelerates adoption. The HITECH Act established meaningful use standards and incentive payments that drove widespread EHR implementation. The HHS Request for Information on AI in clinical care signals continued commitment to technology-enabled healthcare improvement, focusing on cost reduction and outcome enhancement.
But technology alone doesn't transform healthcare. Success requires strategic planning that aligns initiatives with organizational objectives. It demands change management that engages stakeholders and supports adoption. It necessitates security frameworks that protect sensitive health information. And it mandates equity considerations that prevent widening disparities.
The challenges are real—legacy system integration, resistance to workflow changes, budget constraints, and the digital divide all complicate implementation. Organizations that acknowledge these obstacles and address them systematically achieve better outcomes than those treating transformation as purely technical exercises.
Looking ahead, the pace of innovation will only accelerate. AI capabilities will expand into new clinical and operational domains. Internet of Medical Things will proliferate, bringing hospital-grade monitoring into homes. Precision medicine approaches will become standard as genomic sequencing costs continue declining. Blockchain may solve persistent interoperability and security challenges.
Healthcare organizations face a choice. They can view digital transformation as an optional enhancement to traditional delivery models. Or they can recognize it as an existential imperative for remaining competitive, delivering value-based care, and meeting evolving patient expectations.
The evidence suggests only one viable path forward. Digital transformation isn't a destination organizations reach and declare complete. It's a continuous journey of improvement, innovation, and adaptation to emerging technologies and changing healthcare landscapes.
Organizations beginning this journey should start with clear assessment of current capabilities, gaps, and opportunities. They should engage stakeholders across clinical, operational, and administrative domains. They should pilot initiatives to learn before scaling. And they should measure outcomes relentlessly, using data to refine approaches and demonstrate value.
The future of healthcare is digital. The question isn't whether to transform, but how quickly and effectively organizations can adapt to this new reality while maintaining focus on what matters most—delivering high-quality, accessible, patient-centered care.
Ready to begin your healthcare digital transformation journey? Start by assessing your current technology infrastructure, engaging stakeholders across your organization, and identifying high-impact opportunities for improvement. The investment in strategic planning today will determine your competitive position tomorrow.






